Available in Packages/Products: PRESENT Complete Podiatric CME Online
Clinical Examination and Differential Diagnosis of LE Edema
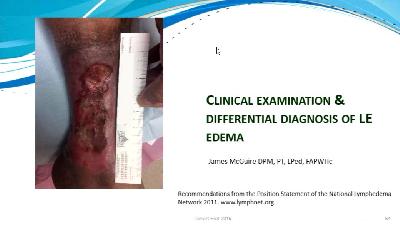
James McGuire, DPM, LPT, LPed, FAPWHcJames McGuire, DPM, PT, CPed discusses lower extremity edema, its clinical presentation and etiology. Dr McGuire recommends specific tests and guidelines to recognize and prevent worsening of the condition.
CME (Credits: 0.75)
Complete the 4 steps to earn your CE/CME credit:
- Complete the Pre-Test
- View the Lecture
- Complete the Quiz (Min. 70% Passing Score)
- Complete the program Survey
- Identify the clinical signs and symptoms necessary to diagnose phlebolymphedema
- Demonstrate an understanding of the differential diagnoses of conditions causing lower extremity edema
- Explain the tests necessary to confirm a clinical suspicion of phlebolymphedema as a cause for lower extremity edema
- Accreditation and Designation of Credits
-
CME (Credits: 0.75)
PRESENT e-Learning Systems is approved by the Council on Podiatric Medical Education as a provider of continuing education in podiatric medicine. PRESENT e-Learning Systems has approved this activity for a maximum of 0.75 continuing education contact hours
Release Date: 03/13/2017 Expiration Date: 06/24/2025
- Author
-

James McGuire, DPM, LPT, LPed, FAPWHc
Director
Leonard Abrams Center for Advanced Wound Healing
Clinical Professor
Department of Podiatric Medicine and Orthopedics
Temple University School of Podiatric Medicine
Philadelphia, PA
- System Requirements
-
To view Lectures online, the following specs are required:
- Broadband Internet
- Browsers must have javascript enabled. Most browsers have this feature enabled by default.
- Any PDF reader. Download Adobe PDF (Free) to print certificates.
Supported Browsers:
- Chrome
- Firefox
- Microsoft Edge
- Safari
Supported Mobile OS:
- Apple iOS 13+
- Android 10+
- Disclosure Information
-
It is the policy of PRESENT e-Learning Systems and it's accreditors to insure balance, independence, objectivity and scientific rigor in all its individually sponsored or jointly sponsored educational programs. All faculty participating in any PRESENT e-Learning Systems sponsored programs are expected to disclose to the program audience any real or apparent conflict(s) of interest that may have a direct bearing on the subject matter of the continuing education program. This pertains to relationships with pharmaceutical companies, biomedical device manufacturers, or other corporations whose products or services are related to the subject matter of the presentation topic. The intent of this policy is not to prevent a speaker with a potential conflict of interest from making a presentation. It is merely intended that any potential conflict should be identified openly so that the listeners may form their own judgments about the presentation with the full disclosure of the facts.
---James McGuire has disclosed that he is on the Speakers Bureau for Smith & Nephew, Osirus, Pure & Clean, Imbed Sciences; has received grant/reaseach support from Reddress and Drexel University; advisory board member for NueEase.


