
The Wound Whisperer
Does Venous Reflux a Venous Ulcer Make?
Does Venous Reflux a Venous Ulcer Make?
A recent paper I wrote was rejected for publication by a vascular surgery publication. The article explained a validated method to stratify venous ulcers by severity (The venous Wound Healing Index). It’s the way that CMS currently allows practitioners to report venous ulcer healing rate under the Merit Based Incentive Payment System. The paper was rejected in large part because the reviewers did not feel that wound care practitioners (of any professional background) could diagnose venous ulcers based on clinical criteria. The reviewers stated that only a venous vascular expert could diagnosis a venous ulcer, and that this diagnosis must be based on venous duplex Doppler scanning.
Here is what the reviewers said when they rejected our paper:
“Many who work in a wound care center have little training or knowledge in how to identify a venous leg ulcer, as opposed to any ulcer... the most important data is the results of an initial duplex scan of the deep and superficial veins for valve reflux, and an ABI. These are the tests that should be done on the first visit to classify an ulcer as venous... The authors appear to be developing an assessment system that will churn patients, spending huge $$ and then referring the patient late to a venous specialist who addresses the problem, after the wound has been initially managed by inexperienced wound care specialists. The alternative and better system is that a patient should initially be evaluated and treated by a vascular specialist before entering a wound care center, not after... The paper seems to be written by authors who have little expertise in venous ulcers.”
That review gave me a good laugh. Wound care practitioners have been diagnosing venous ulcers clinically since the 1800s, long before the advent of venous imaging or venous ablation. There are well known and well accepted criteria for diagnosing a venous ulcer based on patient history and the characteristic of the lesions.
The criteria for diagnosing a venous ulcer include the following:
- Edema
- Hemosiderin deposits
- Lipodermatosclerosis
- The lesions are below the knee and rarely on the foot
- The lesions are well demarcated and irregularly irregular
- Venous ulcers never expose deep anatomical structures
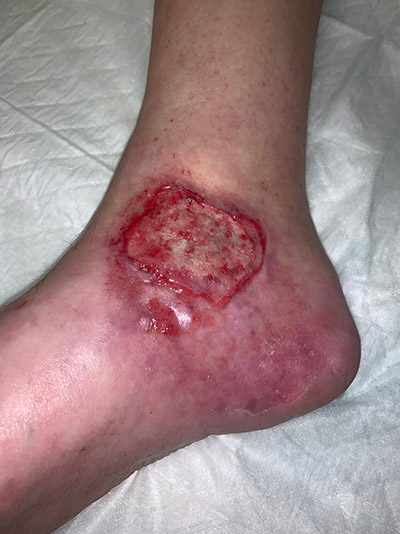
- Venous ulcers never extend below the demarcation line where the plantar fascia attaches (this line is easier to see in dark skinned patients because it is where the pigment ends – see photo with arrows).
If a venous duplex Doppler scan is required to determine whether a wound is venous, then how are we supposed to know who to refer for such tests? That’s actually what the reviewer is saying, which is that ALL lower extremity wounds should be seen by the venous vascular expert FIRST because only they can make the diagnosis.
Just to be clear, I DO refer nearly all of my patients with venous ulcers to a venous expert. I stopped ordering venous Dopplers in the hospital vascular lab except when I’m worried about a deep venous thrombosis (DVT) because the hospital vascular department is only able to look for a DVT. Venous experts do more elegant venous studies for reflux. What makes the most sense to me is to simply refer the majority of patients with venous ulcer on clinical examination. However, I can’t remember the last time I saw a leg ulcer patient in the wound center who had NOT already had an ablation. Many of my patients with active leg ulcers have had several ablations. They keep ulcerating because of all the other medical problems they have, with congestive heart failure being the chief reason. Also, I perform ARTERIAL screening on 100% of my leg ulcer patients on the first visit. That’s the reason I have caught arterial disease that even the venous doctors missed.
Based on the condescending comments made by this anonymous venous expert, I thought I’d have some fun sharing a few cases of non-venous ulcers misdiagnosed by venous experts. I’ve provided photos of patients who were referred to me FROM various local venous experts. These patients had either already had an ablation or were scheduled for one. I think these cases demonstrate that the inability to use long-accepted clinical criteria to diagnose a venous ulcer is not unique to wound care practitioners. Apparently venous experts need some help with this, too. Check out the attached photos of wounds assessed as venous by venous experts (see additional clinical history provided below).
The following patients with leg ulcers were referred to me (sometimes by the vein center) after undergoing venous ablation for documented venous reflux.
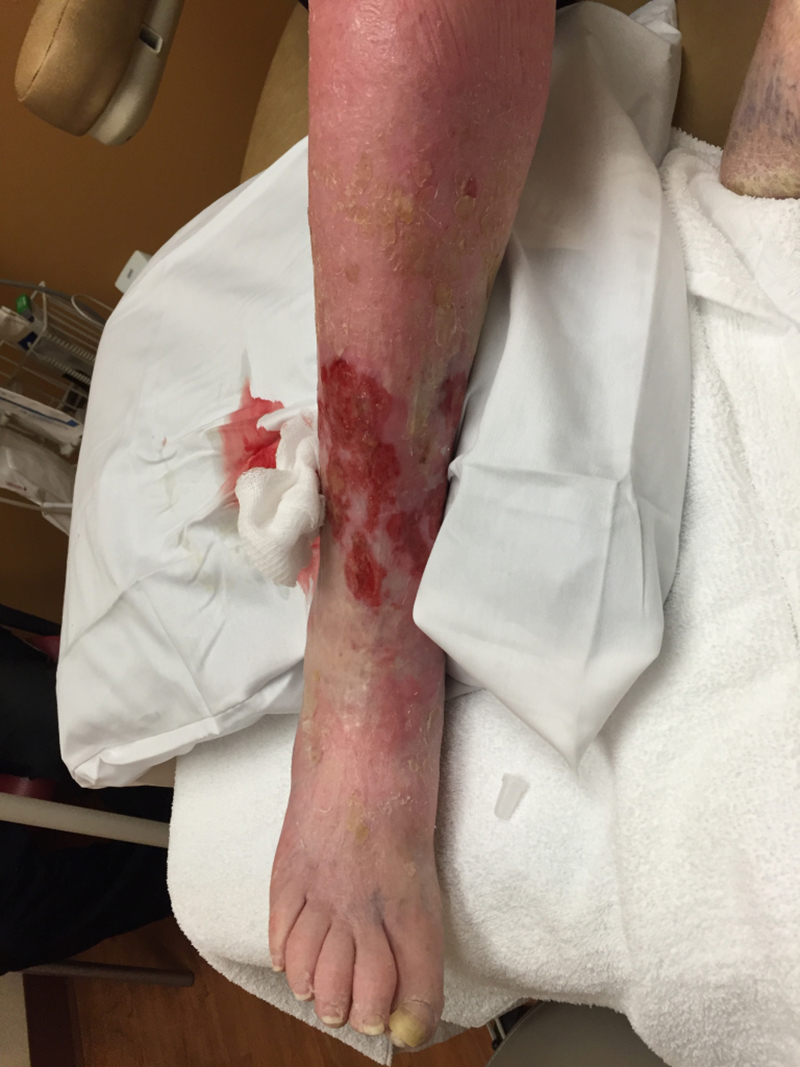
The first is a 92-year-old, alert little lady referred from a local vein center. A circumferential leg ulcer had been present for four years and she had undergone several venous ablation procedures with post procedure compression bandaging, which caused her excruciating pain. She slept in a chair due to rest pain. On her first visit, I performed an arterial screen (a U.S. Wound Registry quality measure). Her skin perfusion pressure was only 18 mmHg (with 30-40 mmHg being the minimum value considered normal) and the pulse volume recording (PVR) on the foot was flat, indicating that she had no pulsatile arterial flow to the foot. I admitted her to the hospital immediately, and the next morning, an invasive cardiologist stented an 85% occlusion of the right iliac artery. What’s the clinical reason these were not venous? The discoloration of her leg is not hemosiderin, but ischemic rubor which begins at the knee due to her very proximal arterial occlusion. The ulcers themselves are not the irregularly regular lesions of venous disease. They are ischemic in etiology.
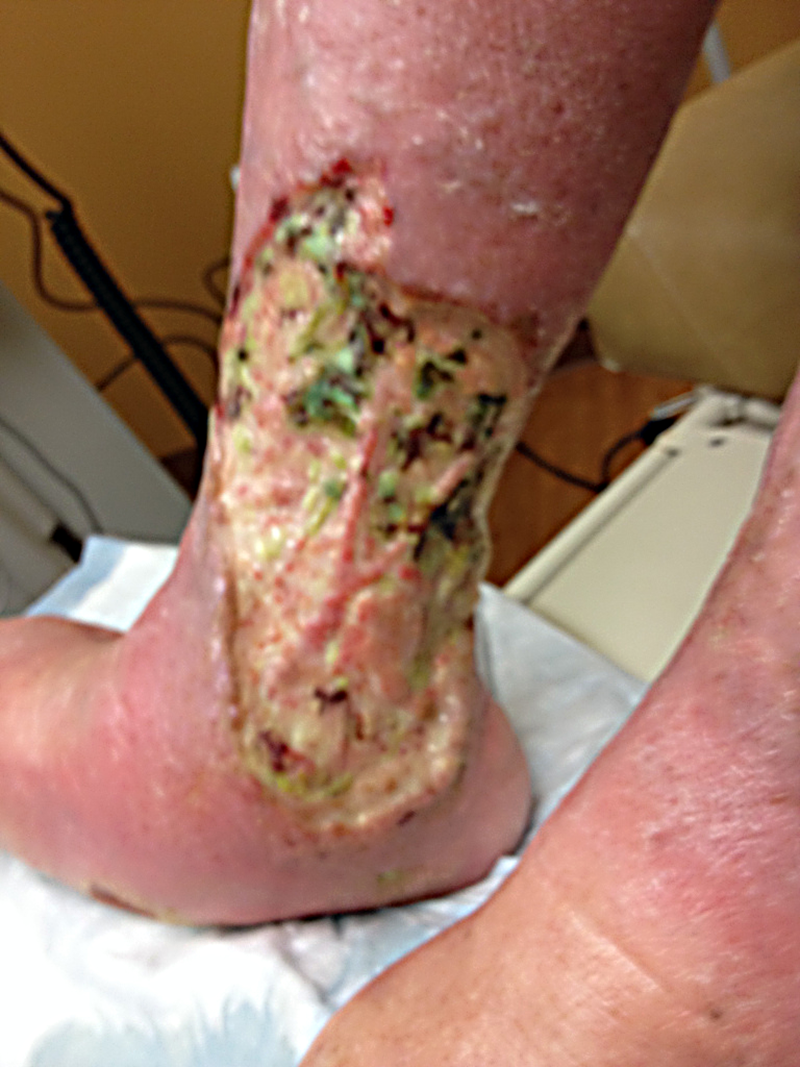
The second patient was also referred from a vein center after undergoing several ablations. Each time they put a needle in him, he got a new ulcer. He has bilateral ulcers that look like this one, which of course, based on their fearful appearance, excruciating pain, and pathergy, are due to pyoderma gangrenosum (the dark discoloration is a Pseudomonas colonization so severe it’s black rather than green). These bilateral lesions cannot be mistaken for venous ulcers since he has deep structures exposed and they are poorly demarcated and extend beyond the demarcation line of the plantar foot. Wrong again, vascular specialist.
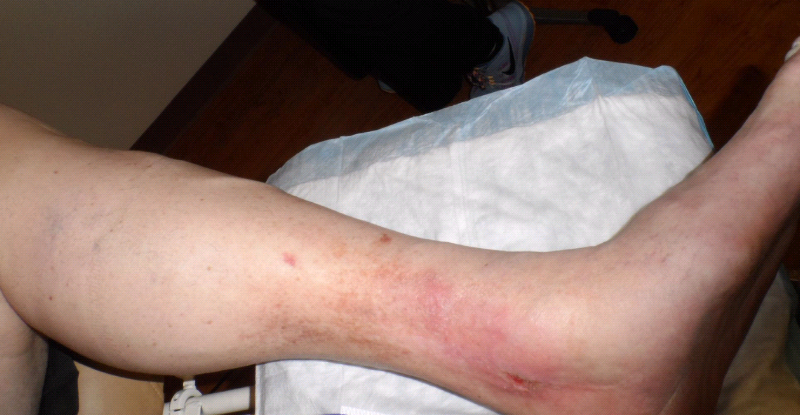
The third case is a retired professional golfer with obvious venous edema and lipodermatosclerosis. He had undergone multiple ablation procedures but failed to completely heal this left medial ankle ulcer despite more than a year of aggressive compression. On his first visit, I was concerned about the texture of his skin and on further questioning, he admitted he had undergone local radiation to the ankle more than 20 years prior. I performed a biopsy which revealed a basal cell cancer and he underwent a very large MOHs excision. Wrong again, vascular specialist. This was a very bad miss.
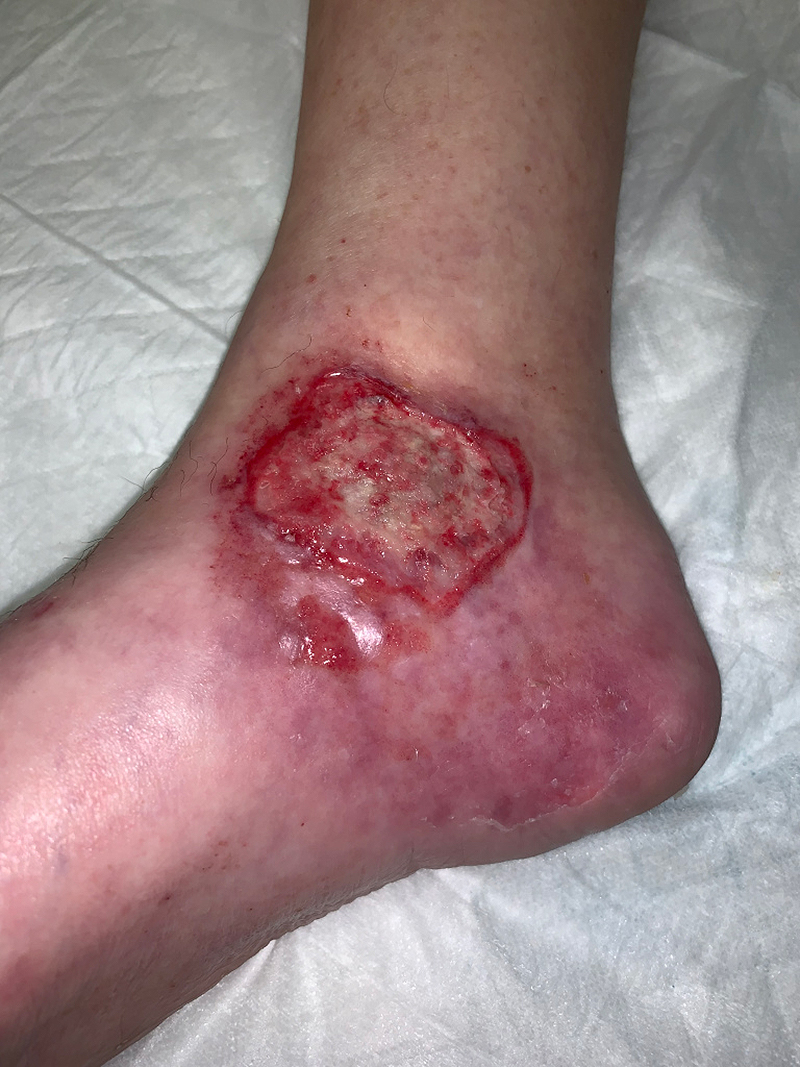
Fourth is a woman with a right medial ankle lesion due to T-cell lymphoma. She has a poorly demarcated lesion that extends beyond the facial attachment.
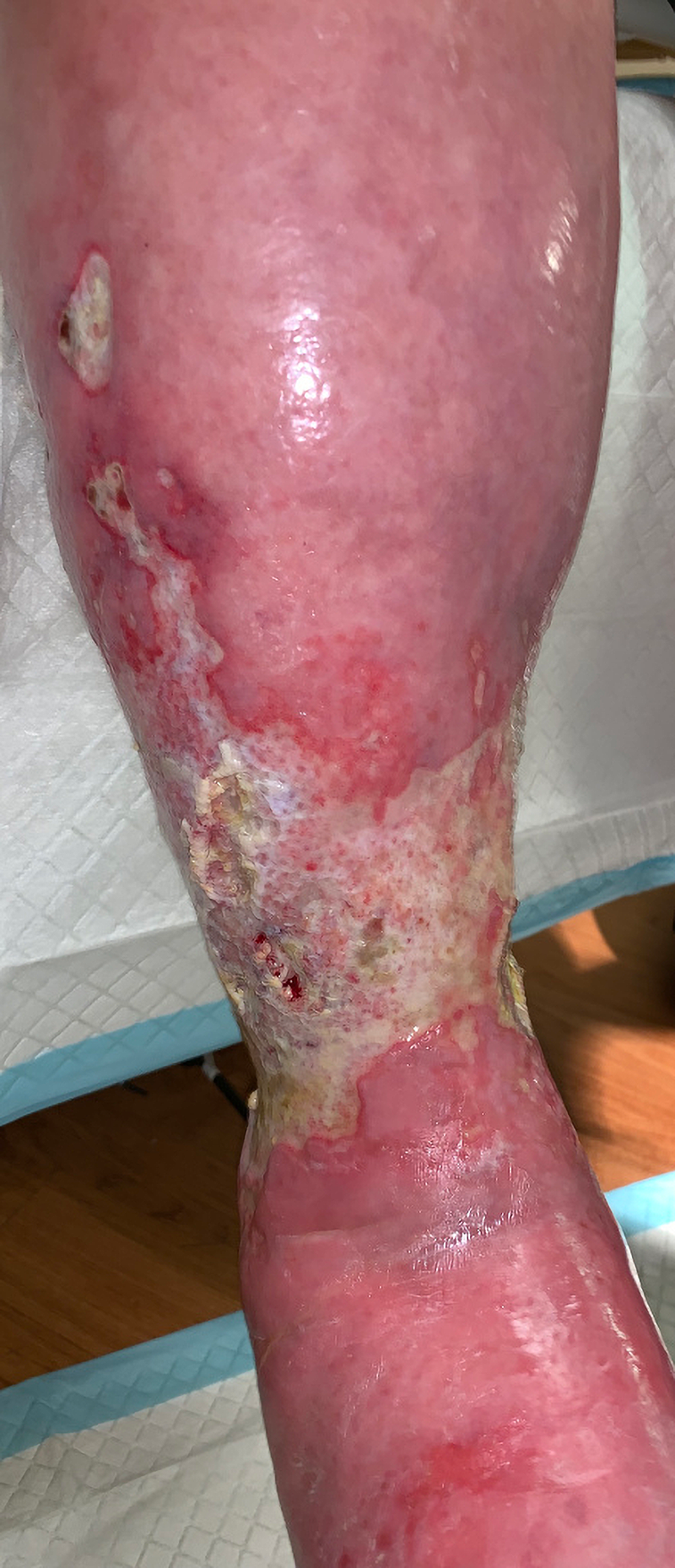
The final patient has polyarteritis nodosa. He has poorly demarcated circumferential ulcers with a purpuric border and he is in excruciating pain. Those findings should have revealed to the venous expert that these were not venous ulcers.
While it may be true that all of these patients have venous reflux disease, they don’t have venous ulcers. Venous insufficiency was not the primary cause of any of these ulcers and treatment of the venous insufficiency alone was not likely to result in improvement. All ulcers among patients with documented venous disease are not venous. I think I just proved that.
Do podiatrists agree that only a venous expert can diagnose a venous ulcer? I’m curious, so I have created a quick survey to find out!
I would like to know if you think it is possible to diagnose a venous ulcer based on clinical criteria? According to the reviewers who rejected my paper, if the ABI does not show arterial disease, and the venous Doppler DOES shows venous disease, we have ourselves a venous ulcer. Since the reviewers agree that I am an inexperienced clinician who isn’t qualified to diagnose venous ulcers, I thought I’d ask the advice of the podiatric community! It is possible to diagnose a venous ulcer based on clinical criteria? Or, if the venous Duplex shows venous disease, and the patient has a normal ABI, does that a venous ulcer make? Let’s vote!
Take a quick survey. It will take you less than 3 minutes and we will report on the results soon>>



Comments
There are 0 comments for this article