
Practice Perfect 670
Biomechanical Decision Making
The KK Approach
Part 3 – Choosing Surgical Procedures
Biomechanical Decision Making
The KK Approach
Part 3 – Choosing Surgical Procedures
Over the last few weeks, we’ve been discussing a method of determining treatment methods for our patients that I’m calling the KK Approach (or kineticokinematic approach). This thought process has us first determine the damaged anatomy, determine the biomechanical underlying cause or contributing factors, and then focus our treatment on those factors. This method is different from the classical biomechanics approach most of us have been taught by deemphasizing simply putting the foot in the right position (the kinematic part) and focusing on adjusting forces about the foot to change function (the kinetic part). Today’s discussion will focus on the surgical side.
The KK approach to foot surgery deemphasizes simply putting the foot in the right position (the kinematic part) and instead focuses on adjusting forces about the foot to change function (the kinetic part).
First, I’d like to point out that the thought process behind the KK approach is exactly the same regardless of whether you are treating a patient surgically or nonsurgically. Again, this is a departure from prior approaches to surgical therapy where the goal was simply to “make the foot straight.” In the past, most of the surgical research was based on comparing measured angles on a radiograph in the preoperative and then postoperative phases and completing some grading method to examine subjective patient outcomes. An example of this is using the AOFAS or ACFAS Foot and Ankle Scoring Systems. The implication behind combining these two evaluation methods was that the improvement in foot position was the cause of the improved patient symptoms.
This assumption may be true, but it is probably not the entire picture. It is more likely that surgical procedures adjust forces about the foot and ankle in much the same way that foot orthoses have been shown to work. To be clear, there is a body of research indicating that the mechanism of functional foot orthoses is not to place the foot into an improved position (ie, subtalar neutral) but rather changing the forces about the foot.1 Surgery most likely functions the same way. The challenge, though, is that it is very difficult to study forces on live patients. We just don’t have the technology yet to measure internal forces and strain on specific anatomical structures. Hence, the growing body of cadaveric literature examining forces and tissue strain.
KK Approach for a Diabetic Foot Ulceration – A Simple Example
With all that as preamble – controversial though it may be – let’s examine a case to demonstrate how the KK approach may be applied to surgical procedure choice. The foot in Figure 1 shows a very common situation: a diabetic foot ulcer - in this case, on the weight bearing surface of the hallux. How would we approach this according to the KK approach if we consider surgical options? The first step is to identify the specific damaged anatomic structure. That’s easy here. The damaged structure is the plantar skin of the patient’s great toe.
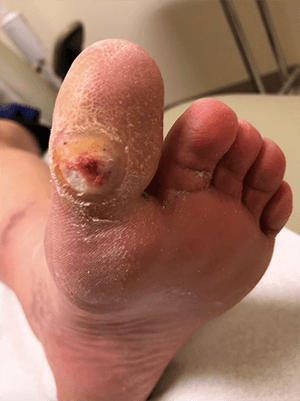
The second step is to consider the factors involved in causing the problem. Again, the biomechanical contribution is not complex. This patient has limited great toe range of motion (hallux limitus), and the lack of movement is compensated at the interphalangeal joint (kinematic contribution). We might also consider other factors such as foot type, decreased ankle range of motion (equinus) and superstructural problems such as knee or leg abnormalities. In this particular patient, those additional issues do not contribute. From this, it is clear that increased plantar pressures have caused the skin to break down (kinetic contribution).
The third step is to address the cause (hallux limitus). Various surgical options might include a hallux interphalangeal joint arthroplasty, great toe joint fusion (with the caveat that compensation for this procedure often occurs at the interphalangeal joint), and the Keller arthroplasty.
KK Approach for More Complex Deformities
The diabetic foot ulcer is a relatively simple example of using the kineticokinematic approach. However, it can also be applied to more complex foot and ankle deformities. The difference, here, is that the biomechanics of complex deformities such as planus and cavus diseases require significantly more research. Additionally, it is imperative for surgeons to know how their choices affect the postoperative extremity rather than simply knowing what plane of deformity it corrects.
Let’s take the medial displacement calcaneal osteotomy (MDCO) as a case in point. Earlier methods of procedure choice would argue the MDCO is for treatment of a frontal plane flatfoot deformity2 or to eliminate the valgus deformity of the heel in order to bring the foot closer to the ideal position.3 A more comprehensive understanding of this procedure would tell us that the MDCO medialized the Achilles tendon4 (creating a more varus pull on the heel bone during gait), an increased ground reaction force medial to the subtalar joint axis (increasing the supinatory torque and realigning the mechanical axis of the limb)5, while decreasing talonavicular joint moments and first metatarsal load and increasing lateral column load.6
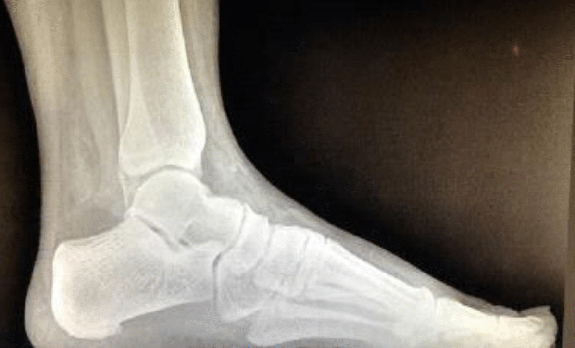
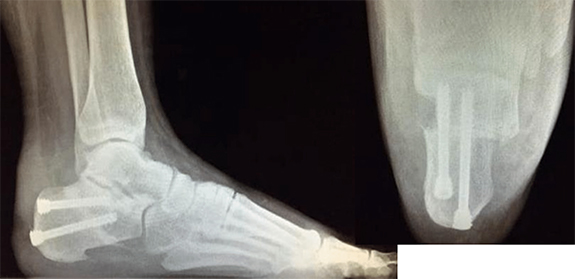
Considering the research in this manner provides a more nuanced understanding of what this procedure offers, and allows the surgeon to choose the procedure based on what he or she wants to do to the foot rather than simply “making it straight.” This approach also leads to other ramifications. For example, if the MDCO medializes the Achilles tendon, creating a supinatory torque (or decreasing pronation), then the practice of performing gastrocnemius recessions during flatfoot reconstructions may need to be abandoned. Why weaken the muscle when it would assist in supinating the foot? In fact, Sung, et al. demonstrated that the MDCO decreased both the Achilles tendon and posterior tibial tendon forces necessary to perform heel rise4 - the actual goal of surgery in patients with posterior tibial tendon dysfunction.
The practice of performing gastrocnemius recessions during flatfoot reconstructions may need to be abandoned, since once you displace the calcaneous medially, the Gastroc complex becomes a supinator…just what you want it to do.
The details that begin to be revealed by approaching our patient’s issues through the KK approach go much further than this article can discuss. Future research should more comprehensively describe both the kinetic and kinematic effects the surgeries we do have on our patients. In that way we will move to a more rational procedure choice and stop focusing on making a straight foot.

-
Huerta JP, Moreno JMR, Kirby KA, et al. Effect of 7-Degree Rearfoot Varus and Valgus Wedging on Rearfoot Kinematics and Kinetics During the Stance Phase of Walking. JAPMA 2009 Sep;99(5):415-421.
Follow this link -
Green DR, Carol A. Planal dominance. JAPMA 1984 Feb;74(2):98-103.
Follow this link -
Root ML, Orien WP, Weed JH, Hughes RJ. Biomechanical Examination of the Foot. Vol 1. Los Angeles: Clinical Biomechanics Corporation 1971.
Follow this link -
Sung IL, Lee S, Otic JC, Deland JT. Posterior tibial tendon force requirements in early heel rise after calcaneal osteotomies. Foot Ankle Int. 2002 Sep;23(9):842-849.
Follow this link -
Steffensmeier S, Saltzman CL, Berbaum KD, Brown TD. Effects of medial and lateral displacement calcaneal osteotomies on tibiotalar joint contact stresses. J Orthop Res. 1996;14(6):980–985.
Follow this link -
Davitt J, Beals T, Bachus K. The effects of medial and lateral displacement calcaneal osteotomies on ankle and subtalar joint pressure distribution. Foot Ankle Int. 2001 Nov;22(11):885-889.
Follow this link































Comments
There are 0 comments for this article