
Paths to Practice Perfection
Best Practice Debridement and the Impact of COVID-19
Best Practice Debridement and the Impact of COVID-19

Debridement is the process in which all materials incompatible with healing are removed from the wound1 and is considered an essential part of wound management. Appropriate debridement undertaken early is likely to accelerate healing, improving patient health and wellbeing and reducing the cost of chronic wound management2. Failure to debride can lead to a range of negative clinical outcomes including, but not limited to, increased risk of infection, ongoing inflammation, abscess formation, compromised restoration of skin function and delayed healing3.
Early evidence on the value of frequent debridement came from a study on diabetic foot ulcer patients. Their data showed that the higher the frequency of debridement the faster the rate of wound healing, and that with weekly debridement, 48% of patients healed in the study period in the test group, compared to only 25% in the control group4. A more recent, retrospective cohort study performed an analysis of nearly 313,000 wounds over a 4-year period. Here they showed that wounds with debridement intervals of 1 week or less healed significantly faster, and this was consistent across all wound types5. Further, in a 25 center study of venous leg ulcers, those centers where frequent debridement was performed had a healing rate of 50% compared to 28% in those centers that performed debridement less frequently, and those that underwent surgical debridement had a 34% higher wound surface area reduction compared to the VLUs that were not debrided at all6. Similarly, a 35 center study on diabetic foot ulcers showed that the healing rate was 30% in centers with frequent debridement and only 13% in centers with less frequent debridement7. Together these findings suggest that regular debridement, at a minimum of once weekly, should be regarded as standard practice for chronic wounds.
However, is there any evidence to suggest that one method of debridement is superior to another? A recent meta-analysis of 14 clinical trials in over 800 DFU patients validated the efficacy of surgical, autolytic and larval debridement, but there was insufficient evidence available to validate the use of either ultrasound or hydrosurgical debridement methods8, presumably due to these being newer technologies that have yet to be fully researched. These results were similar to an earlier meta-analysis9, although in this earlier analysis the investigators did see some evidence that maggot debridement therapy performed better than other methodologies. Together these data support the use of most debridement methods as equal with the major decision factor being clinical and patient preference and cost. More research is clearly needed to validate the use of any one debridement method over another - a point reinforced by a Cochrane review in 201010.
Before Debridement
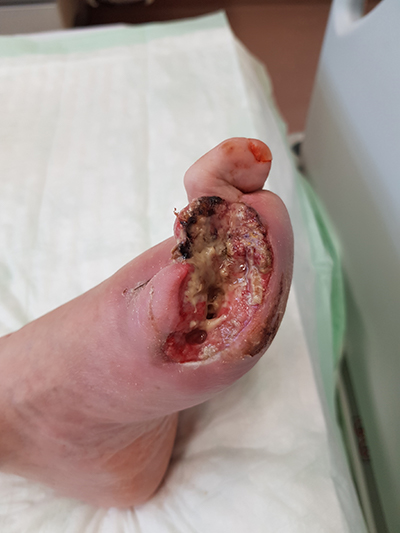
After Debridement

What is the impact of COVID-19 on debridement and wound care?
In the current pandemic situation, CMS has advised that all non-essential surgeries, including wound care, be stopped11 leaving fragile patients without necessary services. This classification of wound care as a non-essential service will result in unintended consequences for patients most vulnerable to COVID-19, leading to increased rates of wound complications and a greater influx of patients into the emergency department12. Given the reduced access of patients to their wound care services, and the well-documented clinical and financial costs associated with a failed or inadequate debridement13, an alternative model for wound care delivery is needed. A very recent paper has proposed a method called Wound Centers Without Walls. This model proposes delivery of wound care to patients utilizing technology and community-centered care where procedures such as surgical debridement and graft placement would move from the hospital inpatient or outpatient setting into the physician’s office or even the patient's home14. It remains to be seen as to how wide spread this Wound Centers Without Walls practice of wound care will become, however given the likelihood of the current situation extending well into 2021, it may offer the best approach to offering debridement and wound care generally for the foreseeable future.

debritom+: Strong debridement for the OR and mild-moderate debridement options for the outpatient setting. The Micro Water Jet technology of debritom+ provides the power of choice for wound debridement across the full continuum of care.
To learn more about debritom+ visit https://medaxis.ch/us.html
-
Cornell RS, Meyr AJ, Steinberg JS, Attinger DE. Debridement of the non-infected wound. J Vasc Surg. 2010 Sep;52(3 Suppl):31S-36S.
-
Jones ML. Should necrotic wounds always be debrided? Wound Essentials. 2015;10(2):26-29.
-
Vowden K and Vowden P (2002). Wound bed preparation. World Wide Wounds.
Link here. -
Steed DL, Donohoe D, Webster MW, Lindsley L. Effect of extensive debridement and treatment on the healing of diabetic foot ulcers. Diabetic Ulcer Study Group. J Amer Coll Surg. 1996 Jul;183(1):61-64.
-
Wilcox JR, Carter MJ, Covington S. Frequency of debridements and time to heal. A retrospective cohort study of 312 744 wounds. JAMA Dermatol. 2013 Sep;149(9):1050-1058.
-
Cardinal M, Eisenbud DE, Armstrong DG, Zelen C, Driver V, Attinger C, Phillips T, Harding K. Serial surgical debridement: a retrospective study on clinical outcomes in chronic lower extremity wounds. Wound Repair Regen. 2009 May-Jun;17(3):306-311.
-
Marston WA, Hanft J, Norwood P, Pollak R. Dermagraft Diabetic Foot Ulcer Study Group. The efficacy and safety of Dermagraft in improving the healing of chronic diabetic foot ulcers. Diabetes Care. 2003 Jun;26(6):1701-1705.
-
Elraiyah T, Domecq JP, Prutsky G, Tsapas A, Nabhan M, Frykberg RG, Hasan R, Firwana B, Pro- kop LJ, Murad MH. A systematic review and meta-analysis of debridement methods for chronic diabetic foot ulcers. J Vasc Surg. 2016 Jan;63(2 Suppl):37S-45S.
-
Tian X, Liang XM, Song GM, Zhao Y, Yang XL. Maggot debridement therapy for the treatment of diabetic foot ulcers: a meta-analysis. J Wound Care. 2013 Sept;22(9):462-469.
-
Edwards J, Stapley S. Debridement of diabetic foot ulcers. Cochrane Database Syst Rev. 2010;CD003556.
-
Centers for Medicare and Medicaid Services. (April 7, 2020). CMS Adult Elective Surgery and Procedures Recommendations: Limit all non-essential planned surgeries and procedures, including dental, until further notice.
Link here. -
Alliance for Woundcare Stakeholder Position Statement. (March 20, 2020).
Link here. -
Cregan MD. (2020). The value of a good debridement.
Medaxis white paper available here. -
Rogers LC, Armstrong DG, Capotorto J, Fife CE, Garcia JR, Gelly H, Gurtner GC, Lavery LA, Marston W, Neville R, Nusgart M, Ravitz K, Woelfel S. Wound Center Without Walls: The New Model of Providing Care During the COVID-19 Pandemic. Wounds. Epub April 24, 2020.
Link here.


Comments
There are 0 comments for this article