Allergic Contact Dermatitis: A Review
Neil Patel and Deon Guduru (2nd year students at Temple University School of Podiatric Medicine in Dr Tracey Vlahovic’s Fundamentals of Dermatology Class), edited by Tracey C Vlahovic, DPM (Clinical Professor, TUSPM)
You’re hiking in the woods with some friends. You brush across a tree with 3-leaved vines wrapping around it, but at the time you don't think much of it. Some time passes by and you notice a strange rash on your arm that itches like crazy. Congratulations! You now have a rash most likely caused by an allergic response to poison ivy.
Allergic contact dermatitis (ACD), is a type of eczematous skin rash which occurs approximately 14 to 21 days after being in contact with certain allergens. These can be anything from, “adhesives, topical antibiotics, fabrics, clothing, fragrances, cosmetics, soaps, moisturizers, nail polish, hair dyes, hair perms, nickel and poison ivy”.1 The delay in onset of symptoms occurs since this disease is a form of Type IV delayed, cell-mediated hypersensitivity reaction. Allergens initiate a response in skin T cells, sensitizing the patient. Continued exposure or re-exposure will lead to cytokine release by memory T cells in the dermis (formed from the previous exposure) and an inflammatory response will ensue. The process of sensitization itself takes 10 to 14 days.1
The amount and duration of exposure will decide the course of the disease, ranging from acute to chronic forms. The acute form presents with redness of the skin, swelling, vesicles and itching. In addition, we may see some crusting and oozing of tissue.1 In the chronic form of ACD, the skin becomes lichenified (increased presence of skin lines), fissures may appear, and areas of well-demarcated pigmentation may present.
Clinically, ACD presents with erythema and pruritus which eventually may progress to lichenification and fissuring in chronic cases. The inflammatory response can be triggered by any given allergen, and it can lead to spread from the original site of contact with the allergen. For example, individuals that are allergic to nail polish could have a rash appear on their face from scratching with a polished fingernail. ACD has similar features to Irritant Contact Dermatitis (ICD), making it difficult to distinguish, so a patch test would help differentiate between these two skin issues. A patch test exposes various allergens to the upper back and is checked in 48 hours to see if there is any erythema, edema, or vesicles that persist under the allergen filled chambers. “Physician office applied patch tests may involve allergens tailored to the patient’s history (Finn Chamber, SmartPractice) or the commercially prepared most common allergens (T.R.U.E. Test®, SmartPractice and allergEAZE, SmartPractice).”1 “In the case of shoe dermatitis, one can use a piece of the patient’s shoe or an extract of the chemicals from the shoe on non-involved skin to elucidate the cause.”2 With this specific test, one could deduce the offending allergen in the setting of ACD. Once the allergen has been identified, it must be removed from the patient’s environment.
Podiatric Significance
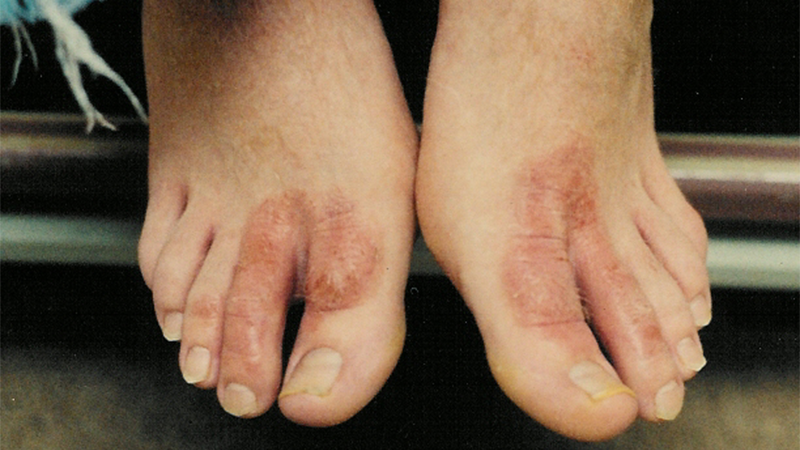
Foot dermatitis due to an allergic reaction to sock or shoe material is an issue you are bound to encounter in the field of podiatry. Patch testing is necessary to find which of the possible allergens from shoe gear are the source: potassium dichromate (dyeing of leather shoes), p-tert butylphenol formaldehyde resin (adhesives and glues used in shoe making), cobalt chloride (seen in leather as well), and mercapto mix and MBT(rubber in shoes).3 Dimethyl fumarate is another common anti-humidity component seen in socks, and can cause allergic contact dermatitis in susceptible patients.
Treatment for foot dermatitis involves prompt removal of the offending allergen and a treatment plan involving anti-inflammatory topicals. Therapy varies depending on the severity of ACD. Once the allergen has been identified and removed, most patients need minor supportive care in the form of topical corticosteroids and prescription moisturizers. The moisturizers help reduce transepidermal water loss, while the corticosteroids help reduce inflammation and itching involved with the disease. “Thicker ointments are generally favored over creams, and bland petrolatum is less likely to cause sensitization compared with the preservatives and emulsifiers found in creams.”3 In some instances, oral steroids (prednisone) may be prescribed if there is a severe reaction.“In addition, hypoallergenic shoes/socks or custom materials that don’t involve the shoe allergen in question must be discussed with the patient.4,5 Ultimately, treatment of this eczematous reaction involves investigation to find the source of the rash, pharmaceuticals to ease the patient’s symptoms, and a plan to keep the allergen out of the patient’s environment in order to prevent recurrence.
References:
- Vlahovic T. Keys to Diagnosing and Treating Contact Dermatitis. Podiatry Today. 2016 Oct;29(10):54-59
- Matthys E, Zahir A, Ehrlich A. Shoe allergic contact dermatitis. Dermatitis. 2014 Jul - Aug;25(4):163-171.
- Bangash HK, Petronic-Rosic VM. Acral Manifestations of Contact Dermatitis. ClinDermatol. 2017 Jan - Feb;35(1):9-18.
- Corazza M, Baldo F, Ricci M, et al. Efficacy of New Barrier Socks in the Treatment of Foot Allergic Contact Dermatitis. Acta Derm Venereol . 2010 Oct;91(1):68-69.
- https://www.dermasilk.co.uk/





Comments
There are 0 comments for this article