
Practice Perfect 728
Logic Prevails: A Case in Point
Logic Prevails: A Case in Point
This case presentation is for our resident readers. Attendings, you’ll see why in a moment. I recently saw a 50-year-old patient in the hospital who was admitted for right lower extremity cellulitis. I find cases like this very instructive for new learners as far as how to approach case workups and the thought process for such in a logical manner.
This diabetic female had a long-standing history of chronic venous disease with a prior endovenous repair. Over the last few days, she noted increased redness and swelling to the right lower extremity. She denied constitutional symptoms. She was under care from another provider who was applying an emollient cream to the leg and she was not wearing her previously prescribed gradient compression stockings.
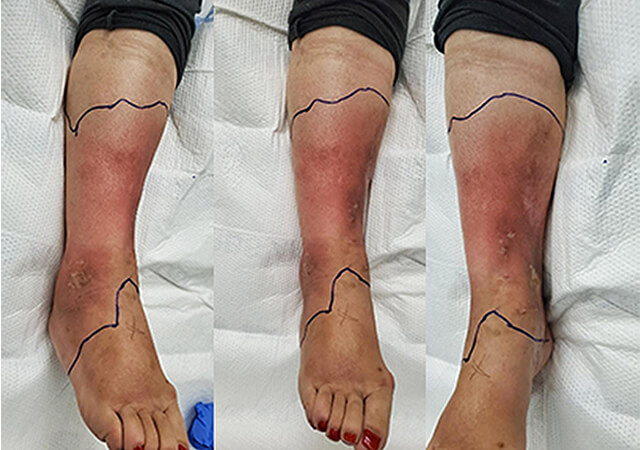
In the emergency room, she was noted to have the right leg appearance noted in the images below. You can clearly see the erythema distal to the midleg which spares the foot. There were no ulcers, but she had multiple islands of hypopigmented scarring from prior wounds. The erythema improved significantly with elevation of the limb. Her pulses were palpable. Her vital signs were normal and labs that were drawn in the ER showed an 11,000 white blood cell count. All other labs were normal. She was admitted to the hospital and placed on intravenous vancomycin and piperacillin/tazobactam.

Does this patient have lower extremity cellulitis?
If you define cellulitis as “inflammation of the subcutaneous layer of skin” then I’d say yes. However, if you define it more commonly as “infection of the subcutaneous layer of skin”, then I’d argue the diagnosis is incorrect. My diagnosis for this patient is acute venous stasis dermatitis with chronic venous insufficiency. My proper care for this patient would not have been IV antibiotics but rather leg elevation and compression therapy.
Teaching Points
This is a great opportunity to consider some different points for resident education.
- As consultants, we are expected to make our own diagnoses rather than just parrot the admitting diagnoses - Those of us in practice who do hospital work have seen this type of situation more times than we can count because the medicine service doesn’t understand venous disease as well as podiatry. This is yet another reason why podiatrists are important members of the healthcare team.
- A logical thought process - will bring us to the proper diagnosis, avoiding the red herring that is a diagnosis of infection. This patient with a history of venous disease presents with no signs of infection other than a red, swollen leg. Her vitals and labs are benign. Most importantly, there are no open lesions on the extremity. For those of you who still think this could be an infection, my question to you is this: how would an infection enter the tissue? As we all know, there are three ways for an infection of the lower extremity to occur: hematogenous, direct inoculation, and contiguous spread. In the adult diabetic, the first two are remarkably rare causes, and if this patient has no entry point, then how would she have an infection? More logically, this patient with chronic venous disease is having an exacerbation.
- Infection vs Inflammation - Recall that the body has only so many ways to respond to any insult. Remember those cardinal signs? Calor, rubor, dolor, tumor, functio laesa. Same signs for infection as for inflammation. So, it makes sense that this patient’s red, warm leg will look like it’s infected when it’s not.
As always, nothing replaces a detailed and comprehensive history and physical. Sprinkle some logical reasoning on top of that and you have the makings of a solid diagnosis to provide that high-quality care to your patients.


































Comments
There are 0 comments for this article