
Practice Perfect 735
Communication During the COVID-19 Pandemic
Communication During the COVID-19 Pandemic

One of the challenges with being a caregiver of any type is empathizing with our patients beyond our normal interactions. Some people do this better than others, and at one point in our lives, we all become patients. However, our loved ones’ entry into the healthcare system provides an important opportunity for us to learn lessons we might not have otherwise, and to become better physicians in the process.
Recently, a family member’s illness required hospitalization. The details of the hospital admission itself are not important, but the situation and challenges involved are very pertinent to our discussion. My family member spent approximately one week in the hospital after being admitted through the emergency room. During that time no one was allowed to visit, and this caused significant strain to the rest of the family.
First, there’s the obvious loneliness and social isolation for the patient. They’re stuck in the hospital, a foreign environment for most nonmedical people, without familiar faces and the comfort of the usual. I’ve increasingly seen patients utilizing technology, especially texting and video teleconferencing, to mitigate this problem. It doesn’t replace the touch of a loved one, but it helps.
Second, it is incredibly difficult to obtain information about the family member and remain informed of their care. These barriers to communication create a huge wall between the family and hospital, with the family dealing with the agony of the unknown.
There isn’t a great solution to this problem because it is clear that social distancing is a very important measure to prevent spread of the pandemic. However, there are ways to mitigate these challenges.
- Let’s recognize the importance of nurses - These professionals spend the most time with the patient, and they are a key intermediary between the isolated patient and the family. We must understand, though, that nursing is a very difficult job both physically and mentally, so we must always remain cognizant of the risk of burn out. Where possible, I would suggest to hospitals to give their floor nurses a designated time period of one hour per day dedicated to communicating with family rather than taking calls on the move. Other nurses would temporarily cover for a nurse during this time. Clearly, this requires more staff, which may not be possible in certain parts of the country already strained by high COVID-19 numbers.
- Hospitals should increase patient advocacy and social work programs - These professionals can be utilized to communicate with patients and their families while making sure privacy is maintained. As an example, it is always helpful for providers to know who has medical power of attorney and who the proper emergency contacts are. Oftentimes the patient’s facesheet information is not the same as the best family contact. Having professionals better able to focus on this would create a communication pathway between family and hospital that would benefit both sides.
- Doctors need to maintain stellar communication - Physicians are the primary decision-makers in patient care, and they also have the most medical knowledge and experience. As a result, doctors are positioned to play a key role not only in leading the medical team but also in communicating with both the patient and family. They also seem to be the first members of the care team to forget their key role as communicators. For all doctors, I recommend the following: If you do a surgery, call the designated family contact immediately after surgery. When you complete a consultation on a hospitalized patient, make it part of your protocol to call the family before leaving the hospital. Give yourself extra time to do this. When possible, use teleconferencing technology in the room with the patient present to efficiently communicate with the family.
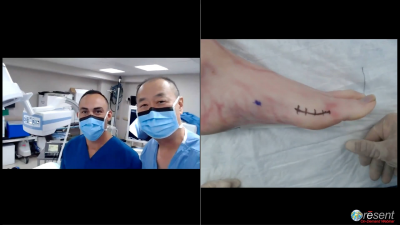
When possible, use teleconferencing technology in the room with the patient present to efficiently communicate with the family
During rapidly changing situations, realize one may need to call family more than once in a day.
One’s tone of voice, calmness, and professionalism will make the difference between anxiety and fear on one hand and measured acceptance and satisfaction on the other
Finally, don’t forget to be gentle. Terrible things may be happening to their loved one, and one’s tone of voice, calmness, and professionalism will make the difference between anxiety and fear on one hand and measured acceptance and satisfaction on the other.





























Comments
There are 0 comments for this article