
Practice Perfect 760
The Optimal Operating Room
The Optimal Operating Room
One can imagine that writing a weekly online blog for the past 16 years might create some challenges finding topics. As a result, my wife – my partner in all things (really my better in everything) – often supplies ideas and suggestions for topics. Easily, I can consider her my muse. And in regular form, she recently emailed me an article from the New York Times called Operating Rooms Go Under the Knife.
This interesting report discusses ways in which hospitals are bringing in multidisciplinary teams to re-examine and re-imagine our ORs with the goal to modernize and upgrade their capabilities. I found the idea of the article intriguing, but I was disappointed at the lack of creativity in the “re-model” ideas discussed. It described increasing space to handle new technology such as intraoperative MRI (I love the idea of real-time intraop CT scans) and using the ceiling for things such as mounted booms with equipment. It reviews green lighting to help with vision when the lights are turned down and discusses a “modular” approach to the use of ORs and ICUs to accommodate changing needs, though never actually describes what the modular approach actually looks like. Yes, these are all good ideas, but when considering the challenges with operating rooms, these changes are appropriate but uninspired. Let’s put on our thinking caps and consider some ideas for the optimal operating room.
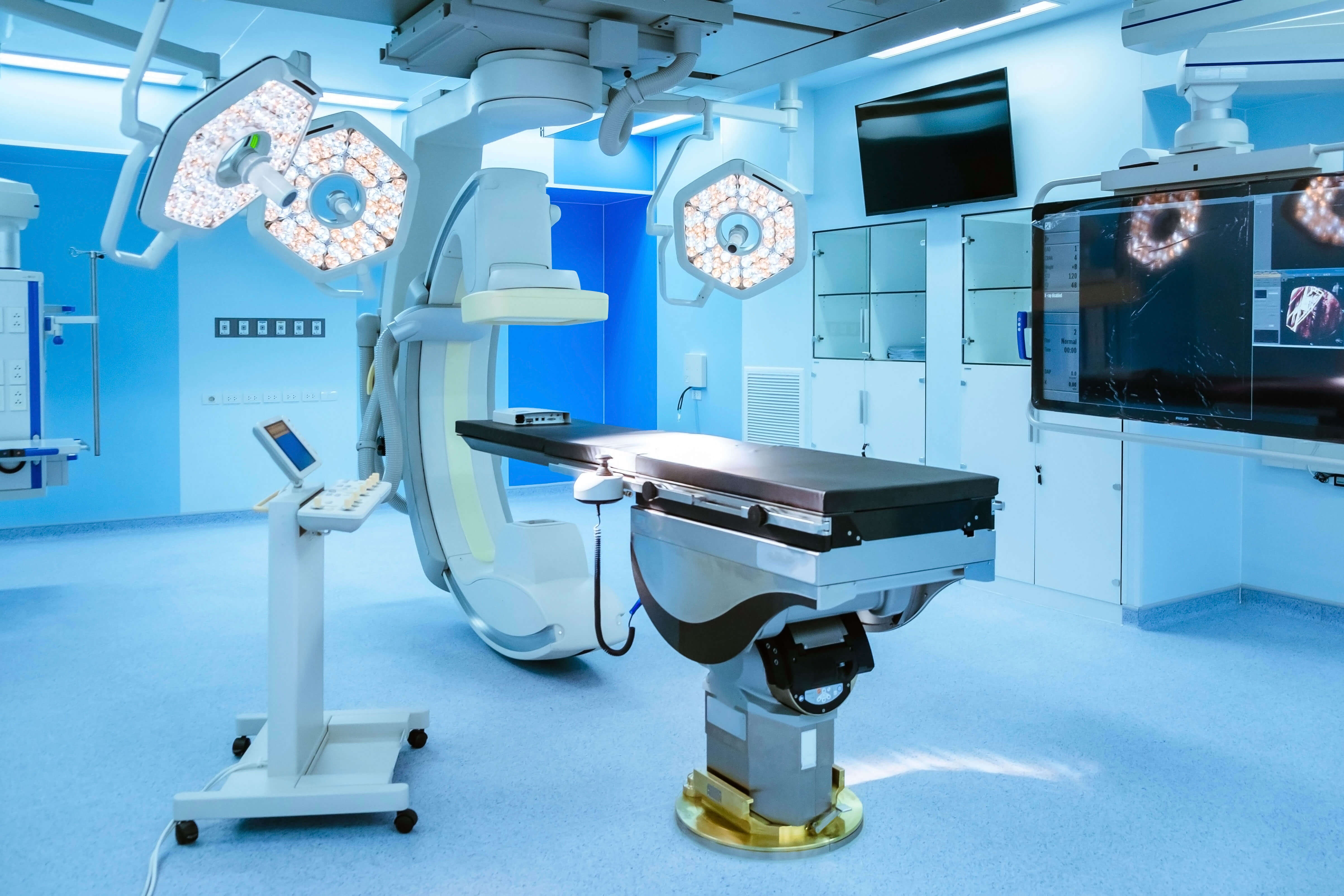
Before we jump into ideas – and I bet each of you have your own, let’s consider some of the current limitations to the modern operating room. It makes sense, then, to focus our modernization efforts on addressing these issues. For reference, take a look at an operating room at one of the more modern facilities where I do surgery.
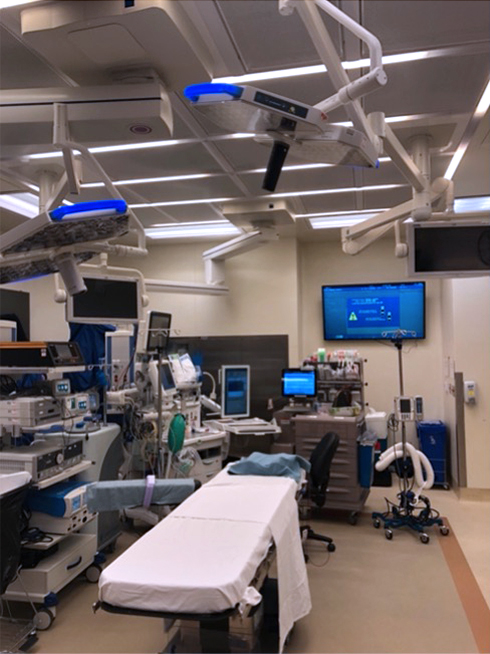

This is a very nice operating room with calm tan colors (rather than white), modern flattop computer screens, and large size. What is not shown are light handles with video cameras installed allowing procedure recording. From my own personal experience this is a luxurious operating room. Let’s talk now about what it, like all operating rooms, lacks.
- Location - All operating rooms are located in a central OR, separated from the rest of the hospital floors. Currently, this is a must. Each OR room must be negative pressurized, for example, which cannot be done in a regular hospital room (not really true – see below). Similarly, there has to be a clean area (behind the red line) to decrease infections. However, this necessity creates its own problems. For example, it takes time to bring patients from their room to the OR – wasted time. Similarly, if a patient is isolated, then they are brought either to an isolation room in the preoperative holding area or straight to the operating room. More wasted time.
- The OR table - The one in the images is the standard table used everywhere. It’s flat, uncomfortable, and inconvenient for many surgeons. Other specialized tables must be brought in for certain procedures such as traction for orthopedics cases or spinal tables.
- Lights - Look at the location of the surgical overhead lights in the images. Where are they located? Near the foot of the bed. One will note that the arms are fully extended, making aiming light at the feet difficult. This requires moving the bed to see the light on the feet, but the bed can only be moved a little due to the fixed location of the anesthesia set up.
- Equipment - Notice the large bank of equipment at the left side of the left image. It is monolithic. Imagine being the circulating nurse trying to maneuver the room. Not shown is the typical large C-arm fluoroscopy system – no different from any other location. Also not shown are the typical patient monitoring methods such as ECG leads that require cables connected to the anesthesia monitors.
- Storage - Not shown is the minimal storage capability in this room. This particular hospital choses to store all of its supplies in a central location. During the procedure the circulator must leave to find what we need – more wasted time, not to mention increased infection risk with multiple door-openings.
I could probably go on with more complaints, and I’m certain every surgeon reading this has a list of their own. Let’s instead move to a conception of the optimal operating room – fantasy though it may be at this time.
First, let’s consider that location issue. It’s definitely a fantasy, but how amazing would it be if we could turn a patient’s hospital room into an operating theater? The door closes, a couple of switches are flicked on and the room becomes negative pressure (much like some current isolation rooms already are). Lights come down from the ceiling (or perhaps the surgeon simply wears a light on their head), and an anesthesia system comes out from a wall closet. The patient’s bed also functions as an OR table (this is definitely possible – I’ve done surgeries on patients in their beds). All major supplies are kept local, so the nurse doesn’t have to run anywhere. Clearly, this is not going to happen in the near future. The logistics to create this are daunting to say the least. But, heck, this is a fantasy, right? True, but if you don’t look for the optimal, you never reach anywhere close.
Sticking with our current centralized operating rooms as they are, let’s think about ways to make them better.
- Make everything cordless - We have the technology now to make cordless devices that use Wi-Fi. Remember those ECG leads I mentioned? Why not make them wireless and set up to communicate with the anesthesia system? How about the cautery system we use? Same thing. Why does it require a cord? For that matter, why do our power saw, drills, and burrs need cords?
- Use the underside of the surgical table - For other devices requiring cords and hoses (think suction and tourniquets), attach the devices to the underside of the operating table so the cords aren’t lying on the floor.
- Miniaturize the equipment - We currently carry smart phones with greater power than room-sized computers used in the 1980s. Why do we need a bank of equipment at all?
- Make it a “smart” OR - In fact, while miniaturizing things, let’s also convert the entire OR to a smart operating room where everything is controlled by a hand-held device carried by the circulator. How about embedding smart technology into the OR bed? It would be nice if the surgeon could control bed height and position themselves along with other parameters, such as the tourniquet.
- Make it mobile - As a result of miniaturization, the entire OR will become more mobile. Remember those lights positioned at the end of the bed? Don’t like that? Turn the table around so the surgeon can place the lights wherever they want. Why does the OR table have to be where it is? Everything is on wheels and yet nothing can move – so they tell us. But we know this isn’t really true. With miniaturization and mobility, we no longer need banks of technology mounted to the ceiling.
- Eliminate the C-arm - As a foot and ankle surgeon, I would be remiss if I didn’t complain about the C-arm fluoroscope. Whether it’s a large C-arm or a small one, I hate both of them. It’s constantly in the way, hard to position, and may require a technician. I’m almost afraid to calculate the number of cumulative hours I’ve lost during my surgeries maneuvering these monstrosities around. Give me a handheld fluoroscope and mobile receiving plate with an image display. This tech actually does exist. We use something similar in the office.
- Change the OR table - Why does this have to be shaped like a bed anyway? Because we sleep on beds? No one does surgery in their bed, so why should the OR table have this shape? How about something adjustable? For heaven’s sake, at the very least make it radiolucent! I’m tired of fighting with the bed.
I could go on forever, as I’m sure all of you surgeons could. Does the optimal OR have to be a fantasy? Well, considering the differences between the modern OR theater and that of the antiquity I don’t think so. What does your optimal operating room look like? Write and let me know. If we receive enough responses, we will publish them in an upcoming Practice Perfect and you can be part of the discussion.


































Comments
There are 0 comments for this article