
Practice Perfect 776
Do Improved Radiographic Outcomes Equate to Improved Patient Outcomes?
Part 3 - The Cavus Foot Evidence
Do Improved Radiographic Outcomes Equate to Improved Patient Outcomes?
Part 3 - The Cavus Foot Evidence
Clearly, I’ve been on a biomechanics soapbox lately. I just can’t get this oh-so-important topic out of my head! Of course, I am a podiatrist, so that makes sense. Over the last couple of weeks, we’ve been discussing an easily overlooked yet fundamental question about the surgical research, which is are improved radiographic parameters indicators of improved patient outcomes? Last week we reviewed a few studies related to adult acquired flatfoot and saw this is in fact the case…to a point. Improving alignment does improve outcomes, but there is a limit to its improvement, and there are other factors at play.
The question for today is, can we apply the same thought process to surgical research about pes cavus deformities? I’ll mention quickly that this isn’t a fair comparison (between flatfoot and cavus deformities) because they are very different entities with different pathogeneses and, in many cases, the goals of surgical treatment are very different. Also, if you look through the literature, you’ll note that it’s very difficult to find surgical studies that examined both radiographic and clinical outcomes. There’s definitely a paucity of research on non-neurological pes cavus. So, with a heavy dose of skepticism, let’s get to it.
Metatarsal and Calcaneal Osteotomy for the Cavus Foot
Sammarco and Taylor retrospectively examined the results of cavus foot surgery in 21 feet.1 Patients with cavus feet of several neurological and non-neurological etiologies underwent a lateral displacement calcaneal osteotomy, lateral and dorsiflexory wedge metatarsal osteotomies (all cases included at least the first metatarsal), and plantar fasciotomy. The researchers reported on preop and postop radiographic and patient survey parameters. They found a significant decrease in forefoot adduction, calcaneal varus, and medial longitudinal arch height as a result of the surgeries. As one might expect, AOFAS Ankle and Midfoot scores doubled. The authors explain the benefits as reducing all aspects of cavus deformity, stabilizing the ankle (though there were no measurements specific to ankle function), and improving gait. It’s fair to say this study argues reasonably strongly that positional changes can be correlated with improved patient outcomes in pes cavus deformities.
Lateral Ankle Instability and the Subtle Cavus Foot
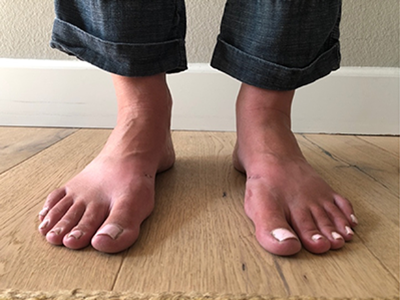
Similarly, a more recent study by Shim and colleagues in 2020 also found improved patient outcomes with specific deformity correction.2 I chose this study because it deals solely with idiopathic cavus, popularly termed “subtle cavus” rather than including neurological disorders. These researchers diagnosed patients with a subtle cavus if they had a positive peek-a-boo heel sign (medially visible heel when looking anterior to posterior with the patient standing) (see Figure 1). They retrospectively examined 15 patients with lateral ankle instability on whom a modified Brostrum along with a 1st metatarsal dorsiflexory osteotomy, Dwyer procedure, or combination of the two were performed. Decision-making for procedure selection was based on physical examination with Coleman block testing and presence of the peek-a-boo sign. They reviewed preop and postop clinical and radiographic parameters as well as VAS and AOFAS Hindfoot scores. Talar tilt, Meary’s, calcaneal inclination, arch height, and hindfoot alignment distance all improved, as did the VAS and AOFAS scores between pre and postop. Again, this study demonstrated a correlation between radiograph and clinical parameters.
The strength of both of these studies is diminished by lack of comparison or control groups as well as the relatively small patient numbers and multiple procedure combinations. But even with these weaknesses, it’s possible to conclude that the improved radiographic parameters do correlate with improved patient outcomes. I may be reaching a bit, but I would suggest that deformity correction in cavus deformities has an even closer connection to symptom improvement. This is likely due to the more rigid nature of pes cavus versus planus deformities. Due to the flexibility of pes planus, there appears to be more room to overcorrect, creating abnormal forces and pressures in the postoperative state. Other differences may be attributed to the mixed neurological and non-neurological disorders in the cavus population, which may affect overall clinical outcomes. The goal for function of a patient with Charcot-Marie-Tooth is arguably not as high as a patient with an otherwise healthy adult acquired flatfoot. Again, this may not be the fairest comparison.
Final Conclusion to Our Question
A more nuanced view shows improved alignment improves outcomes by adjusting forces and pressures about various joints leading to decreased strain on symptomatic structures. Kinematic improvements on radiographs are surrogate markers for improved kinetics but not completely. It appears that it is possible to go too far with these kinematic corrections, more so with planus than cavus deformities, leading to increased joint pressures and strain on new structures, creating new problems. The take home point is to understand the importance of both kinematics and kinetics when it comes to foot and ankle surgery. Truly understanding how each procedure affects the postoperative foot rather than simply aiming for a normalized radiographic angle will lead to better outcomes for our patients.

-
Sammarco GJ, Taylor R. Cavovarus foot treated with combined calcaneus and metatarsal osteotomies. Foot Ankle Int. 2001 Jan;22(1):19-30.
Follow this link -
Shim DW, Suh JW, Park KH, Lee JW, Byun J, Han SH. Diagnosis and Operation Results for Chronic Lateral Ankle Instability with Subtle Cavovarus Deformity and a Peek-A-Boo Heel Sign. Yonsei Med J. 2020 Jul;61(7):635-639.
Follow this link






























Comments
There are 0 comments for this article