
Practice Perfect 645
MRI to Diagnose Osteomyelitis – Know the Details
MRI to Diagnose Osteomyelitis – Know the Details
Nothing in podiatry illustrates the benefit of our profession in the general medical community more than this topic because the devil really is in the details here. Generalist medical doctors like internists simply have too many areas of the body to treat, and the details of highly specialized issues like this are lost. It becomes incumbent on us as lower extremity specialists to make certain that we understand the use of MRI to diagnose osteomyelitis of the foot. To that end, let’s take a look at two quick cases to make sure podiatrists understand those devilish details. We’ll keep our discussion short and high yield, so focus on the take away points from these cases.
Case 1: It’s Just an Ingrown Toenail
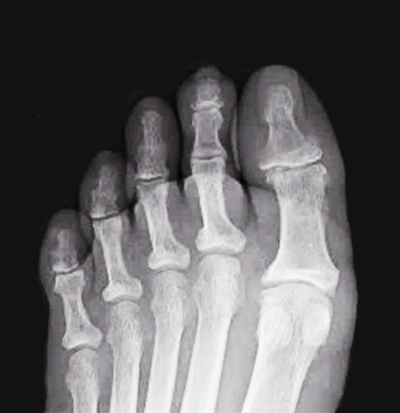
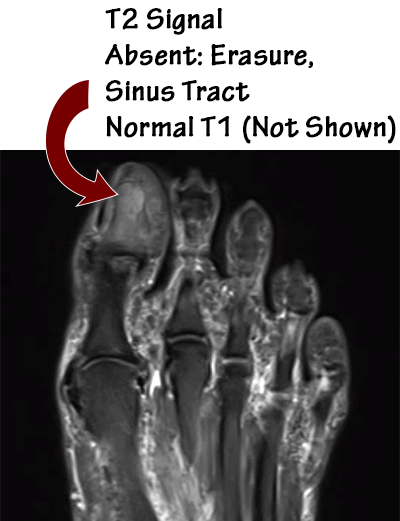
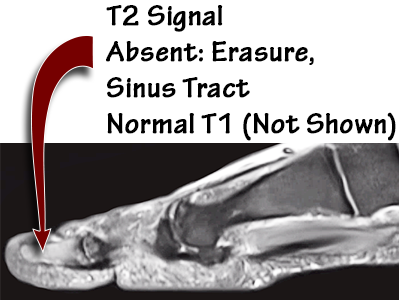
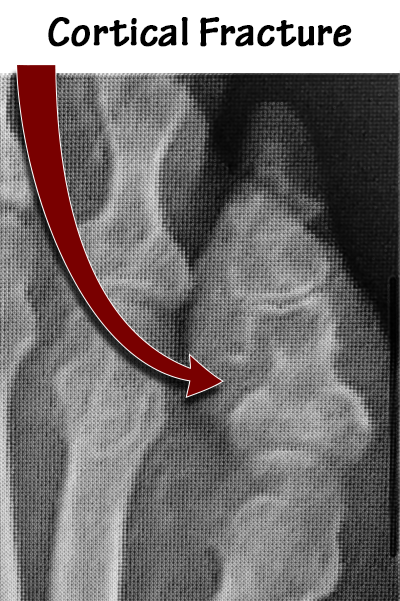
A 65-year-old female was admitted to the hospital after presenting with a red painful swollen great toenail that was actually an ingrown nail. Radiographs and an MRI were ordered (images shown below). Podiatry was consulted, and a partial nail avulsion was performed with complete healing in two weeks. This patient did not have osteomyelitis.
The ability to diagnose osteomyelitis without MRI based on our experience highlights the benefit that podiatrists bring to this critical diagnostic issue
Case 2: It is a Bone Infection
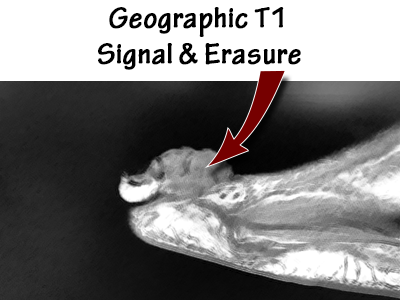
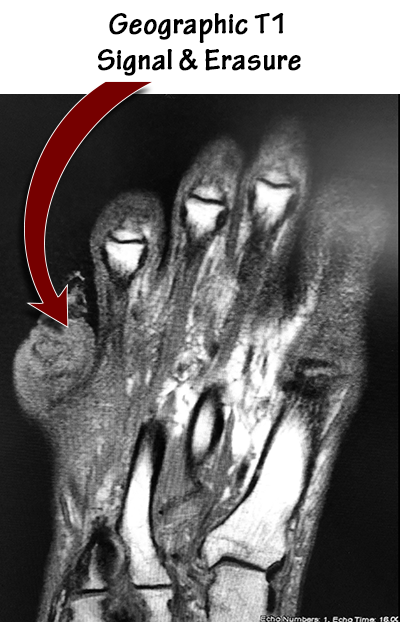
Podiatry was consulted on a 67-year-old male with dry gangrene of the 5th toe. This patient had an ulcer on the dorsal aspect of the digit that probed to bone. Radiographs and an MRI showed classic findings consistent with osteomyelitis.
- Teach your referring providers to consult podiatry BEFORE ordering advanced imaging. Use this as an opportunity to show how important you are.
- There MUST be an interruption in the skin (ulcer, fissure, etc) for there to be osteomyelitis. Hematogenously spread osteomyelitis in the adult is vanishingly rare.1,2
- Radiographic signs of osteomyelitis do lag behind the clinical situation, but when present, there are enough definitive diagnostic tests to guide surgical treatment. Simply put, Ulcer + Radiographic changes = Osteomyelitis.
- Bone biopsy and culture remain the gold standard for diagnosis, but are not necessary in all cases.
- When questions still exist, key MRI findings supporting a diagnosis of osteomyelitis are:
- T1 geographic decreased signal intensity in the bone (a must for diagnosis).
- Loss of cortex in the area of concern (known as “erasure”).
- A sinus tract contiguous with the bone destruction.
- Increased signal intensity on the T2 images. CAUTION – bone marrow edema is highly nonspecific and has several etiologies. DON’T USE THIS TO DIAGNOSE OSTEOMYELITIS IN THE FOOT!
With these diagnostic clues in place, your use of imaging for the diagnosis of pedal osteomyelitis will be more powerful than ever.

-
Bamberger DM, Daus GP, Gerding DN. Osteomyelitis in the feet of diabetic patients: Long-term results, prognostic factors, and the role of antimicrobial and surgical therapy. Amer J Med. 1987 Oct;83(4):653-660.
Follow this link -
Ledermann HP, Morrison WB, Schweitzer ME. MR image analysis of pedal osteomyelitis: distribution, patterns of spread, and frequency of associated ulceration and septic arthritis. Radiology. 2002 Jun;223(3):747-755.
Follw this link






























Comments
There are 0 comments for this article